Using Dry Needling To Relieve Muscle Spasms For SMA Patients

Dry needling has been a popular treatment in the world of physical therapy for the past few years and is continuing to gain popularity with more research being performed. There are many different reasons to use dry needling to improve your patients’ function, with the main reason being to relax a specific muscle and/or muscle group that isn’t responding well to manual soft tissue mobilization.
Within the past few months, our patient with SMA, Michael, began having twitching in his right forearm, specifically his muscles that perform the supination muscle or rotating your forearm where your palms face the ceiling. We began performing deep tissue and trigger point massages to this area, which resulted in relief for the majority of the rest of the day, but the twitching would always return the next day.
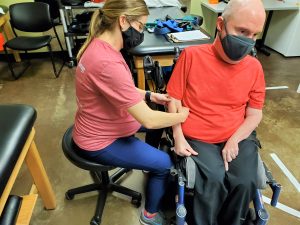

This is the arm that Michael uses during his daily activities, such as manipulating his wheelchair and mouse while working during the day. The twitching became an increasing problem that needed to be addressed. We discussed trying dry needling to test the long-term effects it would have on his forearm, as compared to deep tissue massage. Dry needling is a technique in which a thin needle is placed directly into a muscle, causing it to twitch, and therefore causing the muscle to relax.
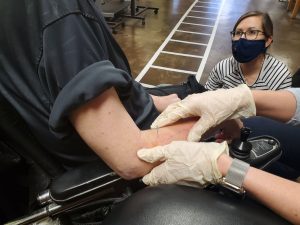
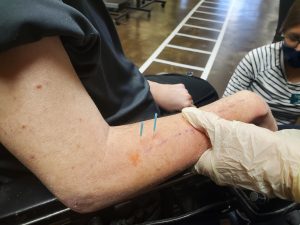
As with any treatment, it is important to rule out any contraindications the patient may have. These include things such as a fear of needles, no consent to perform treatment, history of an adverse reaction to treatment in the past, any medical emergency, or any other reason dry needling may be inappropriate. It is also important to have the patient sign the consent form the lists adverse reactions that may happen such as bleeding and bruising.
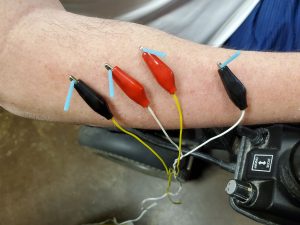
There are different methods of dry needling; some examples include needling with electrical stimulation, the “search and destroy” technique, and interval needling. The first time Michael received dry needling, the therapist used an interval technique where the needles were placed in the trigger points of the spasming muscle. The needles were then allowed to sit in the muscle for a few minutes and were twisted every few minutes to decrease the chance of the needles getting stuck in the fascia. After performing this treatment, Michael had no soreness in his arm and little to no twitching for almost a week. During his last dry needling treatment, he received an electrical stimulation combination, that increased the amount of stimulation to the muscle and theoretically, will increase the amount of relaxation of the muscle.

We will be dry needling Michael every other week for now and will adjust as needed until the twitching has significantly decreased in his forearm. Every week he doesn’t receive dry needling, he will be receiving deep tissue massages to that area as needed.
Michael shouldn’t require these treatments every other week for an extended amount of time. Once this muscle has relaxed, this will be prescribed only as necessary if the muscle or another muscle flares up and causes discomfort or difficulty with his daily activities.
======================== Patient Perspective ========================

When I was a child, I was terrified of needles. I didn’t particularly like them as a teenager either. Now that I’m an adult, let’s just say that I’m used to them. This is probably the same scenario that everyone faces, whether you have SMA, or you are considered able-bodied. Those of us with SMA have probably seen more needles in our lifetime than we ever thought we would, but for me, needles seem to be a necessary part of my life.
I started experiencing these muscle spasms almost immediately when my physical therapists began stretching my right arm and elbow so that I could gain further range of motion. These spasms never really bothered me at the beginning, but as they increased in intensity, they started affecting the way that I was living my life and doing my job.
Constant twitching made it virtually impossible for me to use the mouse on my computer, and it also made it very difficult for me to go to sleep at night. After talking to my physical therapists about this, we decided to give dry needling a shot. Yes, I know, that’s a bad play on words. After listening to some of the benefits that can be achieved by doing dry needling, I decided to give it a chance. Five days after my first treatment, let’s just say that I became a fan of needles.
After my first treatment, the muscle in my forearm didn’t twitch or spasm for five days. When the twitching did return, it was less severe, and only lastly for a short amount of time. I emailed my physical therapist and told her how good my arm felt. She immediately wrote me back and said that she was not only happy that my arm felt better, but she was also excited that the procedure worked because she loved sticking needles in me. Okay, that kinda spooked me, but I quickly remembered that she has the same kind of sick and demented humor that I have.
I just finished my second round of dry needling the other day, and as you can see in the pictures, we used electrical stimulation. During my life, I have had numerous electromyograms [EMGs], but this was different. Instead of the pain that I felt with the EMGs, this electrical stimulation felt as if someone was thumping the muscle. There was no pain involved, and I’m happy to report that a couple of days after this procedure, the twitching and spasming in my right arm has almost been nonexistent.