Increasing Cervical Range of Motion and Reducing Tension For SMA Patients
Cervical, or neck, range of motion is important for many different reasons. A major reason it is needed has to do with safety with scanning the environment during functional activities. Due to scoliosis, Michael has had most of his thoracic and lumbar spine fused, which has limited his range of motion significantly. Considering that his motion has been limited for so long, and with the reduction of muscle mass in his neck and shoulder areas, it may not be realistic for Michael to regain full range of motion, but many different treatments can be performed to help improve his motions, and therefore improve his scanning abilities and reduce the amount of tension that he feels.
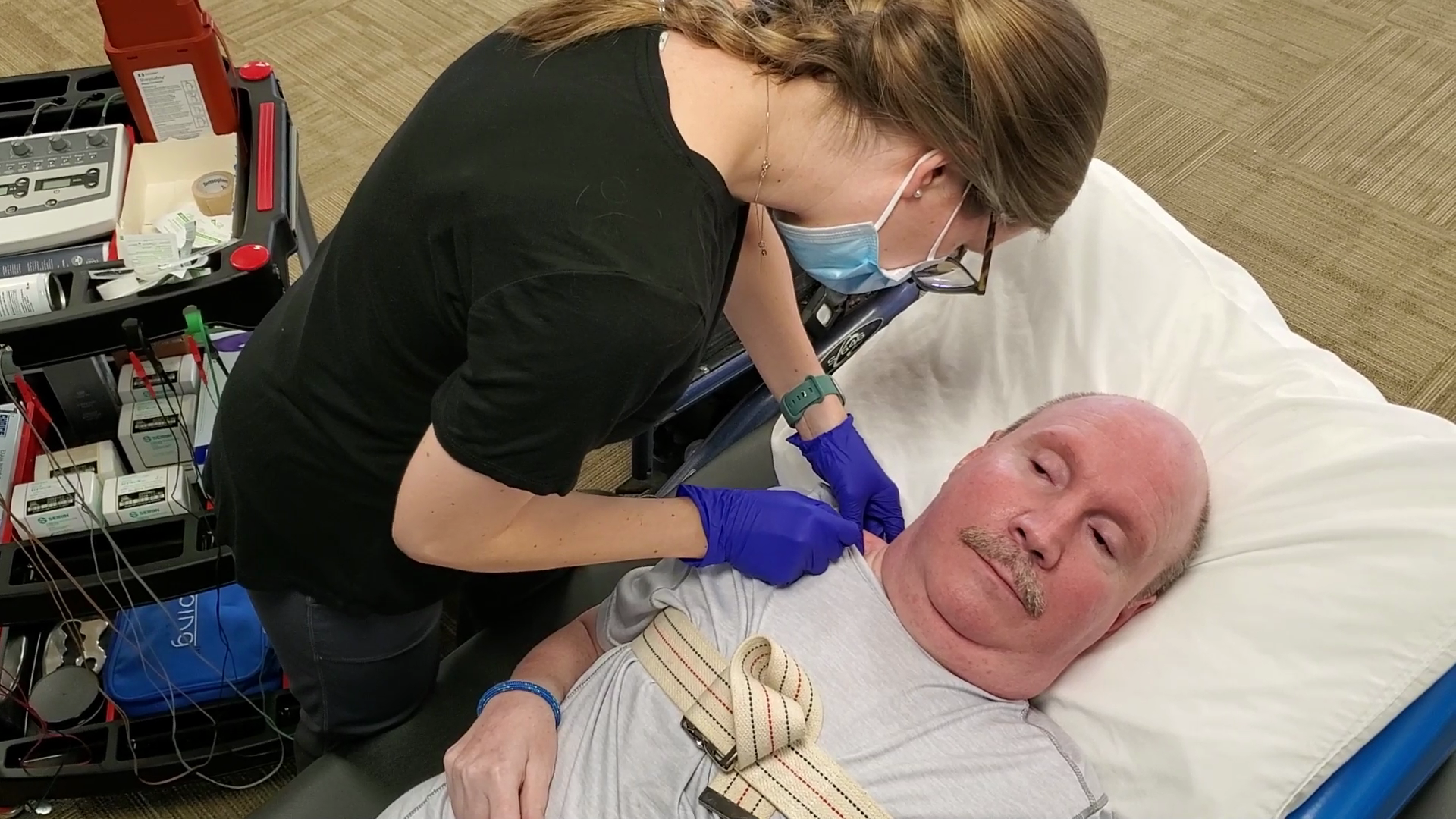
Dry needling, as discussed in previous articles, is used to increase blood flow to the area and allow for reduced trigger points to reduce pain. Michael has received dry needling to his forearm previously and experienced good relief. With this knowledge, we decided to perform dry needling to his upper trapezius muscles. Since Michael is unable to tolerate a prone position for a long period of time, this is performed while he’s in a supine position, which is a safe position. Precautions in this area include avoiding the lungs as well as the subclavian artery and vein. These areas can be avoided by making sure that we stay at least one thumb width above the clavicle as well as avoiding the upper one-third of the muscle and inserting the needle slightly cephalad (towards the head) to avoid these areas. The tissue is grasped above the clavicle and the needle is inserted using in and out motions to elicit a local twitch response to relax the muscle.
We have also tried using soft tissue mobilization techniques to loosen the muscles and allow for an increased range of motion. Due to atrophy in this area, there isn’t a lot of tissue to mobilize which increases the difficulty of performing massage in this area. This is usually performed in a seated position for Michael, secondary to the timing of his treatments and being in his chair every other week while transferring during the off weeks. While this could also be performed in a supine position on the table, there are other activities we perform while on the table that we cannot perform while he is seated in his chair. During the soft tissue mobilization, I use a kneading technique to try and increase blood flow to the area and reduce muscle tension.
Another activity we have performed is stretching his neck in different directions. The main motions we have focused on have been side bending as well as rotation. For side bending, while he is sitting in his wheelchair, I place a hand on his shoulder to stabilize him and use the other hand to perform side bending to the opposite side to increase his side bending range of motion and stretch out his upper trapezius muscles. Next, we work into rotational motions, still stabilizing his opposite shoulder during the motions to reduce compensatory movements.


After these activities, Michael has experienced some increase in range of motion noted with increased ability to scan his environment, as well as subjective comments of reduced tension, felt in his neck and shoulders. All of these activities should be performed on a patient-to-patient basis and making sure to rule out any contraindications to ensure safety for the patient. The main goal, as always, is to improve Michael’s function and comfort during daily activities, not purely just to increase his range of motion numbers for objective measurements. These activities may change throughout the upcoming months depending on how Michael and I feel that his progress is going. There are always modifications and changes that can be made to ensure maximal progression and comfort throughout these activities.



