Improving Muscle Length to Prepare For Future SMA Muscle Targeted Therapy

In preparation for a muscle-targeted treatment, which is currently under development by Scholar Rock for patients with SMA, we have continued to work to maintain the strength improvements Michael has made, but we have also shifted to increasing his range of motion in different joints. In the joints where Michael has contractions, none of them are crucial to his activities of daily living [ADL]. In some patients, stretching is contraindicated because it could further decrease their independence with ADL’s. For instance, a contracture in the hand could be the only way a person is able to grasp the joystick on their wheelchair. With this patient, we would not want to stretch that hand if there’s no indication that function may improve with that hand.
Although stretching itself doesn’t increase muscle mass or strength, it can be a good precursor to working on strength in the future. The more range of motion joints have, the more muscle length the joining muscles have to gain strength in. The idea is to work strengthening in the allowed range, therefore if you have more range, you have more room to work those muscles. With talks of a muscle targeted therapy being developed and eventually approved, the following are some examples of stretches we have been performing with Michael on and off of the physical therapy table while maintaining strengthening exercises to ensure we don’t lose any of the progress we have made regarding his core and neck strength.
Every other week, Michael is transferred to the physical therapy table to work on seated balance, core strength, as well as spending a good amount of time stretching different joints in different positions. While on the table, we start him in a semi-reclined position, as supine isn’t an ideal position for him while stretching his hips secondary to his lumbar fusion, increasing lumbar lordosis while stretching into hip extension. In this position, we work into hip and knee extension simultaneously, with one hand placed proximal to the patella and the other hand on his achilles. In this position, we also use a wedge to work into dorsiflexion. His knee is flexed with the heel on the physical therapy table and digits on the wedge with one hand pressing down proximal to the patella, and the other hand supporting the anterior ankle. Continuing in the semi-reclined position, his hips are stretched into internal and external rotation with hips and knees flexed to 90 degrees. This is also an ideal position to perform the FABERs stretch. Next, we transfer Michael into a side-lying position and stretch out his hip flexors by pulling his hips into extension, while supporting his upper body as well.

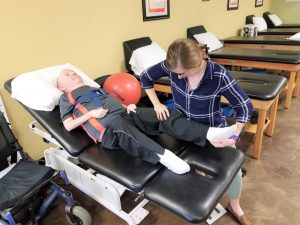
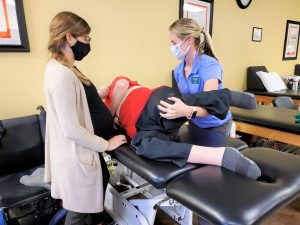
On the weeks we do not transfer him, he still receives stretching in his chair after he performs his strengthening exercises. In his chair, his feet are placed on a wedge on top of a footstool to increase his dorsiflexion, with pressure in a downward motion on his knee and support on his anterior ankle. His knees are then extended with hips flexed and pressure applied proximal to the patella with support on the achilles to increase knee extension and decrease contractures in his knees. While seated, we also work into a seated figure 4 stretch and seated piriformis stretch. We also work on increasing his elbow extension and forearm supination on his right upper extremity, as this is the one he uses for navigating his chair. Michael has also been experiencing some spasms in his brachioradialis muscle that has made it hard for him to work on his computer. For this, he has had dry needling performed on that muscle when needed to decrease the spasms and aid in increasing muscle length.


As previously stated, we will continue to work on improving full-body strength, and increasing muscle length to prepare Michael’s body for upcoming available treatments. We will continue to attempt to prepare Michael as well as we can to increase his independence.
======================== Patient Perspective ========================

Over the past 4 years, physical therapy has provided me with countless benefits, one of which is by increasing flexibility and range of motion. Every one of the physical therapists that I’ve worked with has taken the time to not only learn what SMA is, they’ve also learned how SMA affects me. I count myself as one of the lucky ones because even before physical therapy, my body had not undergone the amount of atrophy and contractures that most patients with this disease have.
Before physical therapy, I was only able to sit in my wheelchair until around 3 PM. My right hip and leg would go numb, and the only way that I could relieve this discomfort was to lay down in bed. Since beginning physical therapy, we’ve worked extensively on my range of motion and flexibility in my hips, knees, and ankles. Now, I can sit in my wheelchair for the entire day without the discomfort that I was experiencing. Before physical therapy, my legs were at a -44° angle, and now, both legs are less than a -20° angle. The benefits of stretching and working on range of motion have far exceeded any benefit that I thought I would receive, and it’s one of the main reasons why I consider myself lucky enough to not only take physical therapy but also have some of the best physical therapists to work with.
There is another potential treatment coming out in the next year, that will specifically target muscle strength and muscle mass. Knowing this information over the past year, my physical therapists have concentrated on stretching and range of motion, so that when this muscle targeted therapy gains FDA approval, my muscles will be longer and more flexible, which will hopefully make it easier for me to start building some of the strength that this disease has taken from me.
If you’re a physical therapist and you get a chance to work with a patient that has spinal muscular atrophy, please take the time to sit with them and discuss the importance of flexibility and range of motion. Do everything in your power to help them to improve in this area. This specific topic of physical therapy is vitally important to not only their comfort level but also will be key to helping them improve their day-to-day lives. Some patients may require aquatic therapy versus land-based therapy, but either way, working on flexibility and range of motion will improve their lives exponentially.