Helping To Control Swelling In Lower Extremities For SMA Patients

Swelling in the lower extremities is a common occurrence in people who are diagnosed with SMA, secondary to different reasons. Some reasons include lack of muscle contraction and the ability to pump fluid out of their feet, as well as positional limitations during the day as most are in a wheelchair for the majority of the day. It is important to decrease the edema to ensure good circulation and decrease other issues that can occur, such as pain and lack of range of motion in the ankles and feet.
There are many different ways edema can be reduced, depending on the person’s mobility and muscle abilities. If the person is able, having them elevate their feet above the heart and performing activities that contract the lower extremity muscles to use their bodies own muscle pump, will increase circulation and recirculate fluids back to the heart. Also, compression stockings are a good way to increase compression more distally, and slowly decrease compression as they progress proximally towards the body to help aid in recirculation of the fluids back to the body. This is one way we attempt to decrease the edema in our patient, Michael, as he is unable to contract the muscles himself to aid in circulation.

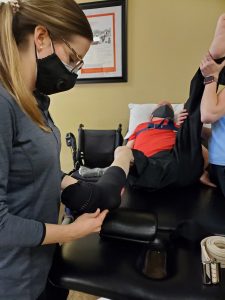
Another way Michael attempts to attack his edema at home is by applying boots that have compression from the feet up to the knees. These boots can be applied for about thirty minutes, to begin adjusting to using them to ensure no abnormal side effects. These compression aids should not be applied if the person has diseases such as congestive heart failure or a known or suspected blood clot, as these could be dangerous with compression.


While in therapy, we can aid in this attempt to reduce edema by performing edema reduction massage. This is performed by elevating Michael’s feet above his heart, and beginning at the proximal end of the swelling, and “milk” the fluid more proximal, and then working more distally to proximally, to aid in recirculating the fluid.
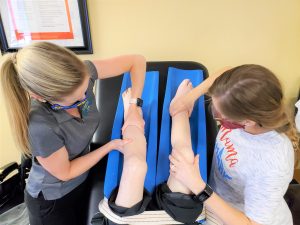
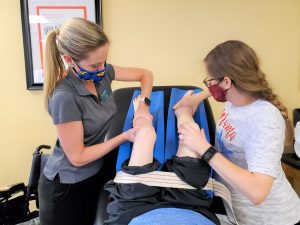
Although it is important to decrease edema in the lower extremities, it is also important to see a healthcare professional to ensure the reason is known for the continued swelling and ensure that compression is a safe treatment prior to beginning any of these techniques.
======================== Patient Perspective ========================

While I’ve always had issues with swelling and edema in my legs, it’s an issue that I never really paid much attention to until I started physical therapy. One of the first things that my physical therapists noticed was the swelling in my ankles and feet, and this was a concern that they immediately started addressing. I sit in my wheelchair, on average, for about 12 to 14 hours each day, and since I don’t wear footrests on the wheelchair that I’m currently in, my legs hang unsupported throughout the entirety of the day. This has resulted in an ongoing issue that needed to be addressed. I recently purchased a new wheelchair, and will soon be sitting in this wheelchair regularly. Unlike the chair that I’m in now, my new chair will have footrests, which will keep the pressure off the underside of my legs and hopefully reduce the amount of swelling and edema that I’m currently experiencing.
Emily, one of my physical therapists, had made a suggestion a few months ago regarding compression socks. These socks provide a constant compression to my feet and ankles, thus helping to push this excess fluid away from my lower extremities. Since the majority of SMA patients do not have the ability to walk, this pooling of fluid can not only become very uncomfortable, it can also be a health concern that the patient will need to address as they age. Over the past few years, the swelling has increased so much, it’s starting to make it very uncomfortable for me to sit for extended periods of time without being uncomfortable. I spoke to my primary care physician about wearing compression socks, and after going in for a physical and a CT scan of my legs, the doctor ruled out any blood clots or aneurysms that could possibly pose any problems. After purchasing a few pairs of compression socks, Emily will put these socks on me each time I go in for physical therapy, and I wear them until I go to bed that evening. Unfortunately, these compression socks are very difficult to put on, but after wearing them for the remainder of the day after my PT session, I can tell that the swelling is reduced, and the discomfort is also much better.
Recently, Emily and I researched and reviewed some compression boots that I could wear for a few hours each night when I go to bed. These compression boots are very similar to the compression devices that hospitals use if you are admitted for any length of time. These compression boots, like the compression socks, push the excess fluid away from my lower extremities. After turning them on, the compression around the top and bottom of my foot activates, and after a few seconds, the compression around my ankles and calves will activate. This movement from the bottom of my foot up through my calves will provide enough compression to move this excess fluid away from my lower extremities. While the compression socks are very difficult to put on each day, the compression boots are very easy to put on and take off each evening when I go to bed. I’ve noticed a big difference in the reduction of swelling and edema, especially in my right foot and ankle since using these compression boots.
I highly recommend that physical therapists advise their patients to consult with their primary care physician before using any compression, like the socks or the boots. The primary care physician needs to rule out any blood clots or aneurysms in the leg that could pose a greater health risk to their patient. Once cleared by their PCP, physical therapists can work with their patients on how to properly use these assistive devices.