Assisted Bridge Exercise Along With Hip Abductor And Adductor Muscle Strengthening (Part 2)
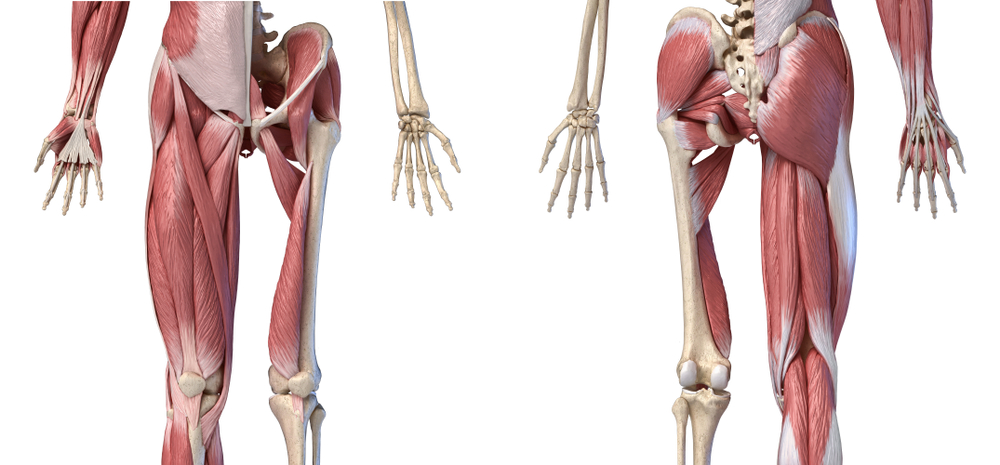
Working with a patient with SMA is not all that different from working with any other patient. Your plan of care advances and changes while working with the patient and making observations as you see fit to the patient’s overall wellbeing. To get Michael positioned for the assisted bridging exercise, where we assist to elevate Michael’s hips while he attempts to contract his glutes to extend his hips, we must roll him side to side to get a sheet under him. While setting up this exercise, there was a discussion of how much control Michael has of his hip abductors and adductors to assist in rolling side to side. With improving the strength in his hip abductor and adductor muscles, Michael will have more control over his lower extremities and be able to keep them in better alignment with less assistance while working on the bridging exercise. This would also allow him the ability to assist more in bed mobility and transfers. The hip abductor muscles include gluteus minimus, gluteus medius, and tensor fascia latae. These muscles work in bringing the leg out away from the body, or abducting. The hip adductor muscles, including gracilis, adductor longus, adductor magnus, adductor brevis, and obturator externus work to bring the leg back in towards the body, or adduct. While we will still perform the assisted bridge exercise with Michael, we have decided that we will also focus on the adductor and abductor muscles in his legs to increase independence in bed mobility and transfers as well as more success in the bridging exercise.
After we lay Michael supine on the therapy table, we position his feet so that his knees will not separate. If his feet are not properly positioned, his hips tend to externally rotate, which is caused from lack of neuromuscular control of his lower extremities. If his feet are in the proper position to where his knees will not separate, Michael does have the ability to abduct his knees with some control. This is the motion we will be focusing on to strengthen his hip abductors. We noticed that Michael had this ability while Laura and I were watching our PT/PTA students work with him this past week. We knew that he had some muscle control, but after testing and applying slight resistance to his legs, we noticed that he did have the ability to utilize these muscles. Over the next few months we will be working with Michael using isometric resistance and possibly resistance bands.
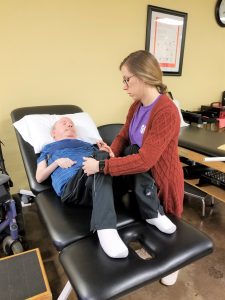
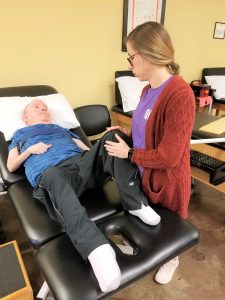
Patients who suffer from SMA, usually do not have muscle control in their legs. Knowing that Michael has trace contractions in these muscles, we can possibly strengthen these muscles to help him not only reposition in bed, but also help him with his balance control while sitting unassisted on the therapy table, along with sitting in his wheelchair on a day-to-day basis.
======================== Patient Perspective ========================

While working with Emily and Laura’s PT students the other day, I noticed Emily and Laura speaking to each other and staring at me with smiles on their faces. When you see your physical therapists smiling at you, and then look away and continue to talk about you, it usually signals the bells and whistles to go off in your head. What are they talking about? Why do they keep staring at me and smiling? Is this going to be painful? Do I need to get up and run away? (Yes, that’s handicap humor, and yes, you can laugh if you want to.)
It would be very easy for Emily and Laura to continue with the same exercises that we’ve been working on for the past 2 years, but both of them have the ability to think outside the box, and by doing this, they’re always coming up with new exercises to help me further my goal in getting stronger. They’re dedication and commitment to making me stronger is something that I wish all SMA patients had with regards to their physical therapists. Most physical therapists have a set of exercises that they do with certain patients, but having the freedom to think outside of the box, has made Emily and Laura more creative in the way that they treat me regarding my physical therapy.
If you’re a physical therapist, and you’re reading this article, please remember to think outside of the box when you work with an SMA patient. What may seem as an unachievable goal to you, may be a dream to someone with SMA, and if you give them the chance to strengthen these muscles, you may be surprised at the results.



